Sun, Citrus & Margarita Burn: Phytophotodermatitis in Summer
Sun exposure after contact with lime or other citrus juices, like from a spilled margarita, can trigger Margarita Burns, causing skin blisters and discoloration.

Welcome to the sizzling sensation of summer, where sun-kissed skies and refreshing drinks are the daily highlight. A beachside escapade with a glass of classic lime margarita brings the perfect picture of a blissful summer vacation. But, did you know that this very beverage that embodies the carefree spirit of summer can add a startling twist to your sun-soaked adventures?
‘Margarita burns’, often disregarded and underestimated, can put an end to the sun-kissed revelry and bring discomfort and pain to even the most seasoned margarita enthusiasts. From blissful sips to painful mishaps, discover the surprising hazards lurking within this tangy delight. We are about to explore the science behind these citrus-infused summer skin sizzlers and equip you with the knowledge to enjoy margaritas safely under the sun.
Science behind Margarita Burns
Scientifically known as phytophotodermatitis, Margarita burns are a type of skin reactions that result when your skin is exposed to lime juice or other citrus juices and then exposed to sunlight or ultraviolet (UV) rays shortly afterwards. This combination can lead to a chemical reaction on the skin, resulting in burns, blisters, redness, and skin discoloration.
According to the paper titled “A spotlight on lime: a review about adverse reactions and clinical manifestations due to Citrus aurantiifolia”, the culprit behind this annoying skin condition is an organic chemical compound called furocoumarin, which is abundant in limes and other citrus fruits.1 They make your skin more sensitive to sun light and UV rays, so you get an exaggerated skin reaction that gives rise to a painful rash. It is called a ‘phototoxic effect’, and it can occur in one of the two ways given below.
- Oxygen-independent reactions, which lead to a disruption of DNA synthesis.
- Oxygen-dependent reactions, which cause harm to different layers of skin: epidermal, dermal, and endothelial cells.
Needless to say, these margarita burns are most common during hot summer days where there is no escape from golden sun rays. Most common scenario is to get this after juicing a fresh lime into your favorite concoction; hence the name ‘margarita burn’ or ‘lime burn’.
It’s not just limes that can cause this, though. Even tequila can be a culprit. Specifically, when you sprinkle salt on your thumb, lick it off along with a slice of lime, and then down a shot of tequila, you expose your skin to the citrus juice, increasing the risk of burns.
Since limes and citrus fruits are used for different purposes like cooking, preparing alcoholic and non-alcoholic beverages, cosmetic uses and essential oils, you better be aware of this summer villain when you engage in any of these activities. Squeezing, cutting or picking the fruit will expose your skin to its juices. Especially if you work as a bartender, gardener or a pastry chef, you are in the high-risk group for lime burns. And this is more commonly seen in young women than in men.1
How to identify Margarita dermatitis
Sometime, there won’t be anything more than a painless dark skin patch.4 But depending on the amount of citrus juices on your skin, length of sun exposure and skin sensitivity of different individuals, this might differ.
You can have a painful red rash with blisters and blackening of the skin. Also, it will appear only in small patches, where you spilled lime or other citrus juice on your skin. They can be in “drip line” patterns or even bruise like hand prints or finger print patterns.
The latter scenario has lead margarita burns to be falsely diagnosed as child abuse, physical violence and accidental burn injuries.2,3
However, the rash will not appear just after exposure to the sun. It usually takes around 36-72 hours to appear.4 It can be hard to diagnose because of this late appearance of symptoms.
There’re three stages in the progression of these clinical symptoms:
- It starts with a red rash accompanied by a burning feeling (stage 1)
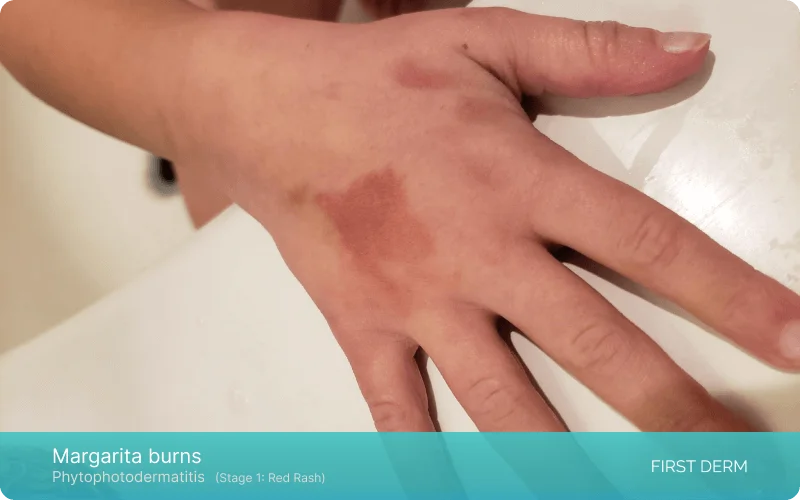
Hand displaying the initial stage of Margarita Dermatitis, also known as Margarita Burns, characterized by mild skin redness/ a subtle red rash
- Followed by painful and swollen blisters (stage 2)
- Eventually, the blisters become soft and lead to darkening of the skin after approximately one week (stage 3).5
The rash usually disappears in a few weeks, while the hyperpigmentation will remain for months after a margarita burn.
Treatment and prevention
Even though it can be frustrating to deal with margarita burns scarring your flawless summer skin, they are often self-resolving and are not dangerous in the long term. So, the treatment is mainly to relieve you from the pain and discomfort.
Applying soothing topical creams or ointments, such as Hydrocortisone creams or aloe vera gel, can help get rid of the symptoms like inflammation, redness, and itching. These products can be obtained over-the-counter.
Over-the-counter pain relievers, such as Acetaminophen or Ibuprofen, can be taken orally to help manage any discomfort or pain associated with the burns. If the burns are severe, widespread, or accompanied by severe symptoms, it is advisable to seek medical attention.
A healthcare professional may prescribe stronger topical medications or provide additional treatments, such as oral steroids or antibiotics, if necessary. When the margarita burn involves more than 30% of your body surface, hospital admission is required in order to manage the wound in the burn units.6
How to protect your skin from margarita burns while enjoying the beauty of summer?
Well, you only have to take some simple precautions:
-
- If you touch or spill citrus juices on your skin, wash it off thoroughly before going outside in the sun.
- It is important to immediately rinse the affected area with cool water to remove any remaining plant residue or juice and minimize further skin damage. Even after rinsing, try not to expose that area to the sun immediately afterwards.
- Wearing sunscreen and protective clothing/hats are good ways to get sun protection.
As painful as these margarita burns sound, you don’t have to let it ruin your summer energy. Just remember about it when you head out to your next summer party, and when you raise your glass, remember to sip responsibly and stay sun-safe.
As we dive headfirst into the carefree days of summer, let’s not forget to bask in the warmth of the sun while protecting ourselves from potential margarita burns. By embracing the sun-kissed moments and treating our skin with caution, we can savor the flavors of those tantalizing margaritas without the unwanted sting.
So, grab your shades, lather on that sunscreen, and let the tropical vibes and cool beverages be the only things you encounter this summer. Here’s to a season filled with endless sunshine, laughter, and margarita-infused memories that leave us with nothing but a blissful, burn-free glow.
References
-
- Alessandrello, C., Gammeri, L., Sanfilippo, S., Cordiano, R., Brunetto, S., Casciaro, M., & Gangemi, S. (2021). A spotlight on lime: a review about adverse reactions and clinical manifestations due to Citrus aurantiifolia. Clinical and Molecular Allergy, 19(1), 1–10. https://doi.org/10.1186/S12948-021-00152-X/FIGURES/6
- Weber IC, Davis CP, Greeson DM. Phytophotodermatitis: the other “lime” disease. J Emerg Med. 1999;17(2):235–7.
- Mill J, Wallis B, Cuttle L, Mott J, Oakley A, Kimble R. Phytophotodermatitis: case reports of children presenting with blistering after preparing lime juice. Burns. 2008;34(5):731–3.
- Fitzpatrick, J. K., & Kohlwes, J. (2018). Lime-Induced Phytophotodermatitis. Journal of General Internal Medicine, 33(6), 975. https://doi.org/10.1007/S11606-018-4315-Z/FIGURES/1
- Maniam G, Light KM, Wilson J. Margarita burn: recognition and treatment of phytophotodermatitis. J Am Board Fam Med JABFM. 2021;34(2):398–401.
- Mateus, J., Silva, C., Ferreira, M., & Porto, J. (2018). Phytophotodermatitis: still a poorly recognised diagnosis. Bmj.Com. https://casereports.bmj.com/content/2018/bcr-2018-227859.short?casa_token=SspxdxzZVQsAAAAA:Hz2tfGd-S9kJol6sUXeqNUbTQm_iSU_EN0F9KqTL7yHW2Ha87W0_-tEO6WkKYjzg_qO7Jzewbj1re8K5CVM
Ask a Dermatologist
Anonymous, fast and secure!

The Specialist doctor from the University Hospital in Gothenburg, alumnus UC Berkeley. My doctoral dissertation is about Digital Health and I have published 5 scientific articles in teledermatology and artificial intelligence and others.

