NetDoctor – Dermatology Artificial Intelligence (AI) test
Can our AI algorithm identify Netdoctor’s dermatology images?
Everyone have used a medical information site like WebMD, Healthline to self-diagnose their symptoms. In Europe there are many, but the most famous one is Netdoctor or Netdoktor in Scandinavian and German speaking countries.
Netdoktor.se is Sweden’s leading health portal with over 2 million monthly visits and 90 000 members. They have medical portal for doctors called NetdoktorPro, which has over 90 000 visits each month and 2 400 members.
The Netdoktor editorial team consists of leading doctors, journalists and web developers who answer members ‘ questions and offer health news, facts and exchange of experiences via forums and blogs. The editorial material is under the independent control of Netdoktor and its medical experts.
It can be difficult from a picture to compare with your skin concern and self-diagnose. We think that skin images search together with an information site like WebMD, Healthline or Netdoctor’s, would benefit immensely for their users if they had some help with artificial intelligence (AI). So we took the example dermatology images of skin diseases and ran it through our skin image search, that gave us top dermatology lesions within a second.
Source: https://www.netdoktor.se/hud-har/
Try our FREE Skin Image Search today and get peace of mind
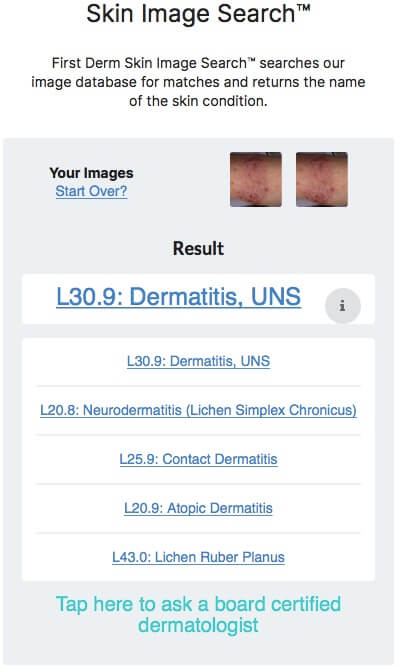
Children’s Eczema (atopic eczema)
Childhood atopic eczema is a long-term, itchy eczema characterized by symptom-free periods of intermediate disease outbreaks of varying severity.
People with childhood eczema have a tendency to have dry skin, low threshold for itching and an increased risk for the developing other types of atopic diseases, like asthma and allergy. Many grow out of their childhood eczema, while others have it continuously more or less throughout their lives.
How do you get childhood eczema (atopic eczema)?
The cause of the disease is unknown, but the risk is higher where more than one family member suffers from childhood eczema, asthma and/or an allergy. Children with eczema often have asthmatic bronchitis, asthma or any other hypersensitivity disorder associated.
The onset is usually begins before the child has reached the age of five years and it is most common at two to six months. More and more children in the Western world have children’s eczema, some theories think it is because we are too clean so the child is not exposed to antigens and can develop their own defense.
Try our FREE Skin Image Search today and get peace of mind
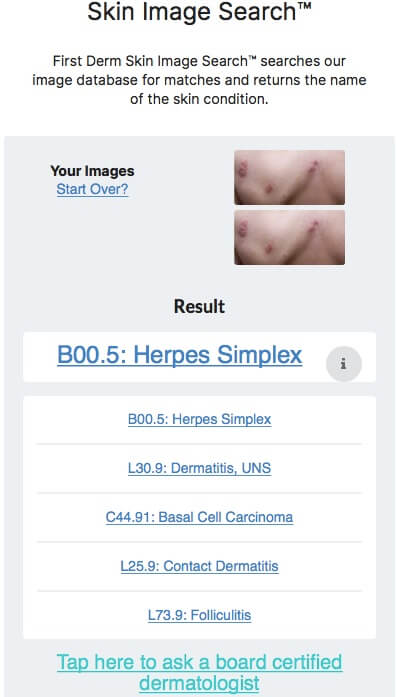
Herpes Zoster vs Herpes Simplex
The result shows herpes simplex, but the image is of Herpes Zoster. This version 33_2 has not been trained with Herpes Zoster images, however version 43_1 can distinguish Herpes Zoster from Herpes Simplex.
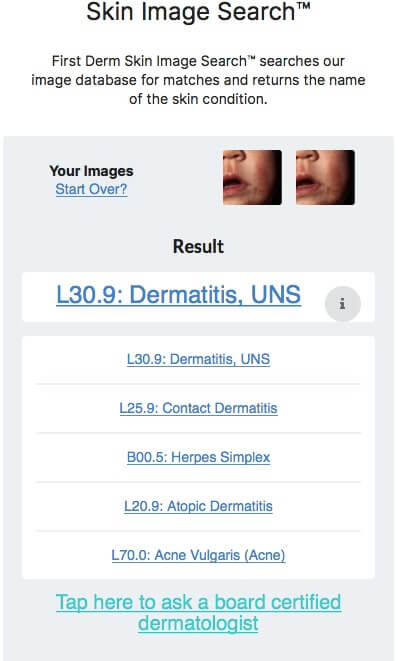
Herpes Simplex (cold sore)
Cold sores are often caused by a very common virus, Herpes simplex virus (HSV), and are characterized by small exuding blisters on a swollen red skin or mucous membrane. The area can be painful and tender. The blisters heal without scarring, but have a tendency to come back at regular intervals.
There are two kinds of Herpes simplex virus where both varieties can attack the skin and mucous membranes all over the body. HSV-1, the most common form of herpes, is usually limited to the mouth and lips. HSV-2 is mainly found on the genitals and has a greater tendency to return.
Approximately 80 per cent of the adult population have antibodies to HSV-1 in their blood. Approximately 25 percent have antibodies to HSV-2.
Try our FREE Skin Image Search today and get peace of mind
Herpes Zoster
Shingles (herpes zoster) is a painful rash caused by the varicella Zostervirus, which also causes chickenpox. Shingles occurs when the chickenpox virus is reactivated, usually many years after the original infection.
Shingles can be transmitted by direct contact with the wound fluid from the blisters, and then gives chickenpox in them (usually children) who have not yet had infection with chickenpox.
What is Acyclovir?
Acyclovir is a medicine used to treat viral infections.
The drug is used in the treatment of infections with herpes simplex virus on the skin and mucous membranes, such as lips and genitals, or in the eyes. Acyclovir may in some cases be used preventively against herpes simplex. Acyclovir can also be used for the treatment of shingles and chickenpox. For the best results it should be taken within 3 days.
Try our FREE Skin Image Search today and get peace of mind
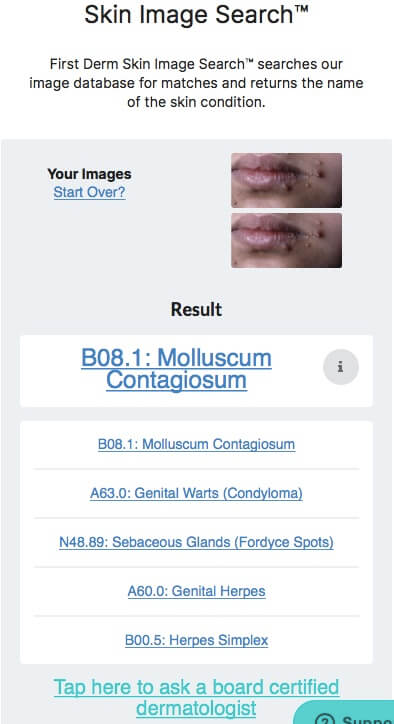
Molluscum contagiosum
Molluscum contagiosum are harmless small round, firm, painless bumps ranging in size from a pinhead to a pencil eraser on the skin caused by a viral infection of the skin’s outermost layer. They are usually 2 – 5 mm in diameter and have a small pit in the middle. It can form everything from a single mollusk to very many and they usually disappear by themselves after six to twelve months.
Molluscum contagiosum are most common in young children and usually sit on the child’s stomach, arms, face or neck. They can also occur in adults and then usually around the genitals, on the lower abdomen and on the upper part of the thighs.
Diagnosis
The rash has a characteristic appearance, which means that the diagnosis in most cases is easy to set.
Cause
Molluscum contagiosum is caused by Poxvirus. They infect by close contact or via objects that may have the virus on them such as towels, clothes or toys, but the risk of infection is small in normal contact. The mollusks can spread to other parts of the body when scratches and takes them. In adults, mollusks are often a sexually transmitted infection.
Try our FREE Skin Image Search today and get peace of mind
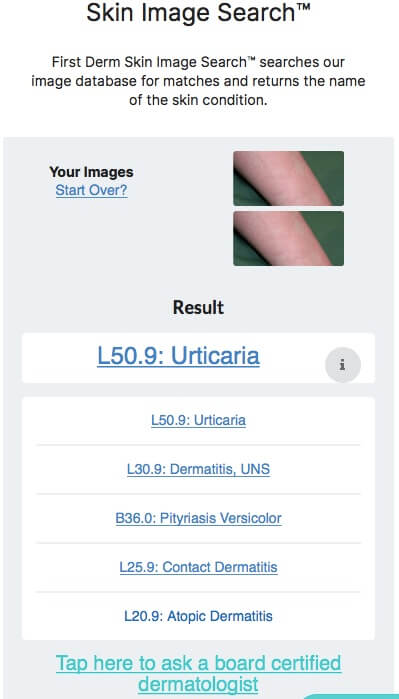
Hives (Urticaria)
Hives is an outbreak of swollen, pale red bumps or plaques (wheals) on the skin that appear suddenly. The rash is similar to that arising from contact with stinging nettles. In Latin, the rash is called urticaria, which comes from the Latin word for nettle (Urtica).
The number of wheals, the size of the wheals and the extent it covers the body varies. The individual wheals occurs and disappears in less than one day, but new can appear elsewhere, in some instances they can last longer than that. Deeper swelling of the skin is called angioedema. Angioedema usually sits on the face, on the arms or legs.
Hives are divided into an acute and a chronic form, and the definition of a chronic hives is that there have been wheals daily for more than six weeks (at shorter time it is called acute). In some patients with chronic hives, the rash is caused by physical stimuli such as cold, heat, sun or grated skin. This form of chronic hives is called inducible hives. The risk of acute hives at some point during liver is about 20 percent, while the risk of chronic hives is about 1 to 4 percent. As many men as women suffer from acute hives, but the chronic variant is twice as common in women as in men.
Causes
Hives are caused by the release of various active substances, including histamine, from so-called mast cells in the skin. These substances allow the small vessels in the leather skin to expand and release liquid to form a local swelling (oedema). In addition, it is formed by this reaction both redness and itching.
Try our FREE Skin Image Search today and get peace of mind
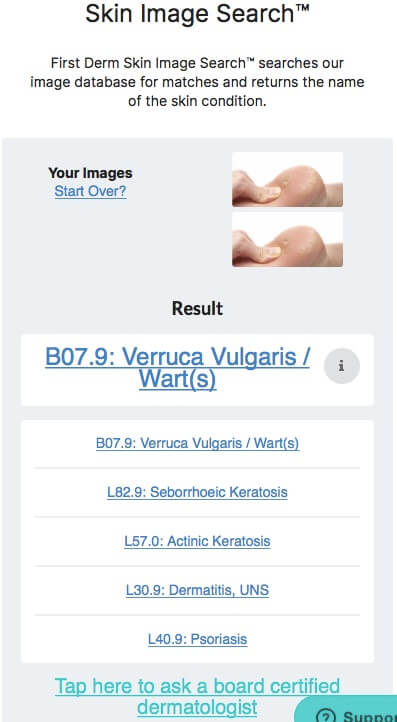
Verruca Vulgaris – Warts
Warts are a viral infection of the skin and they are common on the hands and feet, there are more than 60 different virus strains and only infect people.
Warts are uncommon in children under three years, then increases in frequency. Approximately 5-10% of children between 4-6 years have warts, while 15-20% of adolescents between 16-18 years are affected. The basic attitude is that all children are affected sometime by hand or foot warts. In adults, the frequency decreases rapidly, where warts are associated in people with immunodeficiency diseases or who are being treated with immunosuppressive drugs.
Are warts contagious?
The skin cells where the wart are, release thousands of viruses every day. Warts infect by contact either directly or the cells that have dropped off, it does not effect via the the blood. The risk of infection can be reduced by adding nail polish or plaster on the wart. Warts can also infect indirectly via the floor in the swimming halls and shower rooms.
It may take several months after the infection itself before the warts show up.
How are warts treated?
Warts are treated by self-care to start of with special wart patches.
Try our FREE Skin Image Search today and get peace of mind
Ask a Dermatologist
Anonymous, fast and secure!

The Specialist doctor from the University Hospital in Gothenburg, alumnus UC Berkeley. My doctoral dissertation is about Digital Health and I have published 5 scientific articles in teledermatology and artificial intelligence and others.